
By the time a claim
reaches your adjuster,
the friction is already built in.
It starts at FNOL — where incomplete, inconsistent intake data creates rework, delays, and downstream inefficiencies.
Start with a pilot → prove value in weeks, not years
Bitligence turns unstructured FNOL — voice, text, photos, forms — into structured, decision-ready data before it reaches your adjusters. Built for mid-size carriers. Governed by design.
Built by someone who processed 20,000+ FNOL calls a day at a national carrier. This isn't theory.
Not ready to talk? 👉 Try our ROI Calculator first
Built Specifically for Mid-Size Carriers
Get to production AI — without a 12-month implementation, a data science team, or a seven-figure commitment.
The hardest part of claims AI isn't the model. It's the mess that comes in before it.
Bitligence focuses on FNOL, where manual effort is highest and data quality issues begin.
We run structured pilots on your real intake workflows. Measurable improvements in speed and data quality — within weeks, not quarters. No disruption to your existing systems.
Built on real claims experience — not experimentation.
See what a focused FNOL pilot looks like for your operation.
Trusted Claims Intake AI — From First Notice to Confident Decision
Most carriers fix claims problems downstream. We fix them at the source — at intake, where the data quality is actually set.

Step 4: Risk
Early Fraud Signal
Detection
Surface fraud indicators at intake — before they become costly investigations.
Most fraud signals exist in the intake data. Bitligence surfaces them at first notice — quietly, consistently, and before costly investigations begin.
• Pattern detection across claim narrative, loss details, and policy data
• Consistency checking between claimant statements and coverage records
• Risk scoring at intake — flags routed to SIU before assignment
The best time to catch a fraud signal is the moment the claim comes in.
Step 2: Documents
Claims Document
Intelligence
Stop letting key information sit trapped in documents.
Claims come with policies, estimates, notes, records, photos, and reports. Bitligence extracts, validates, and structures that information automatically so it becomes searchable, comparable, and ready for decision-making.
• Automated extraction from policies, estimates, photos, and reports
• Cross-document validation — flags inconsistencies before they cause rework
• Full audit trail — every extraction logged, explainable, and reviewable
Every document. Structured. Searchable. Auditable.
Step 3: Decisions
Triage & Risk
Signals
Route the right claim to the right adjuster — the first time.
Bitligence uses structured intake data to power routing, severity classification, and complexity scoring so each claim moves to the right queue from the start.
• Severity scoring and complexity classification at intake
• Adjuster matching based on claim type, workload, and skill profile
• Early identification of claims requiring specialist handling
Catch the complexity early. Route it right the first time.
Governance — Built In, Not Bolted On
The Trusted AI Layer
Across Every Step
Every decision. Explained. Logged. Audit-ready — from intake through routing.
Governance and compliance controls aren't an add-on. They run underneath every workflow, so when a regulator asks why a claim was prioritized or flagged, the answer is already there.
See FNOL AI in a Real Claims Workflow
AI agents capture, validate, and structure claim intake — turning unstructured inputs into decision-ready data in real time.
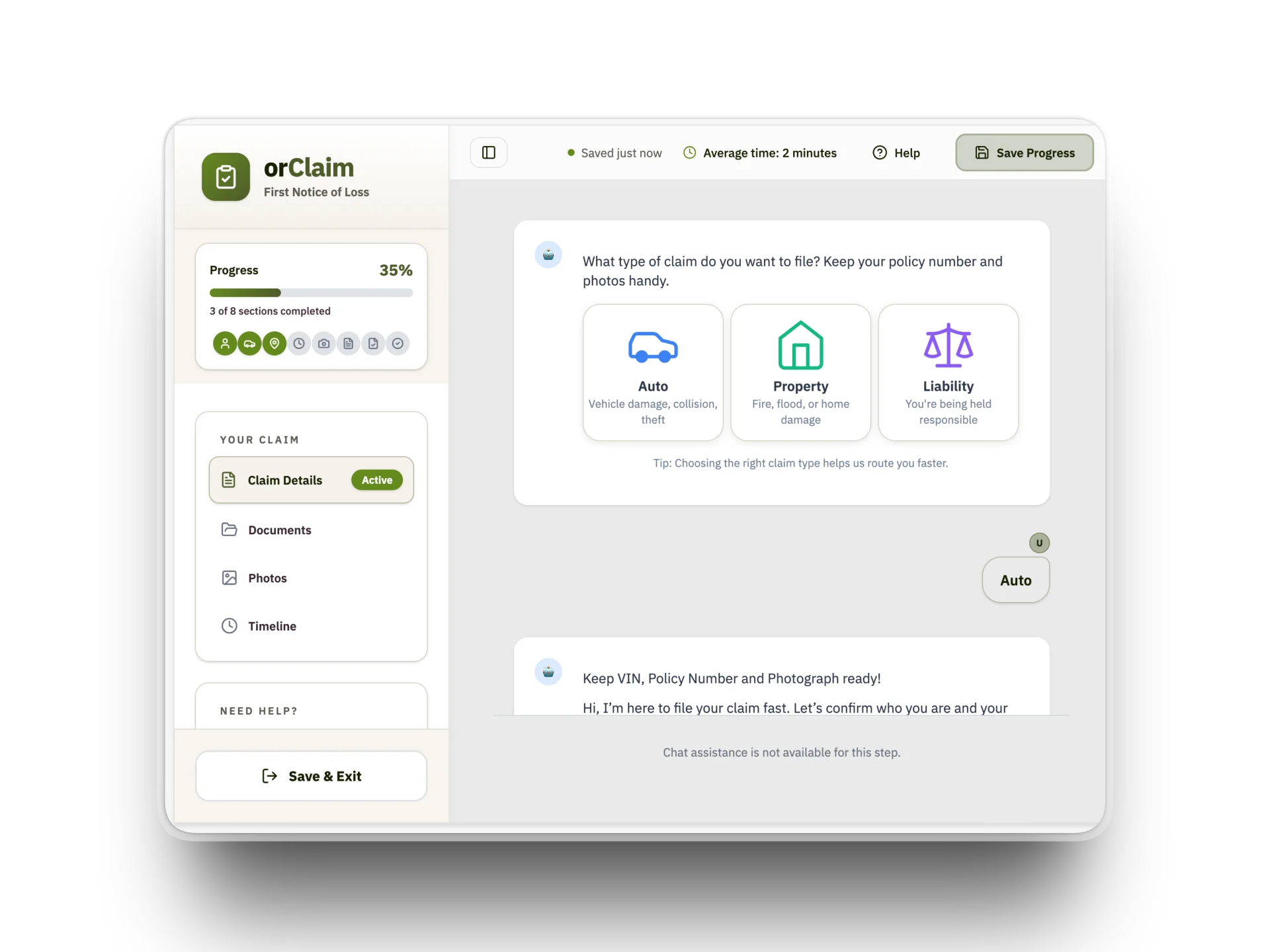
From Messy FNOL to Decision-Ready Claims
What actually changes when intake is structured from the start.
Before
Unstructured FNOL
Emails & Messages
Updates scattered across inboxes — no single source of truth
PDFs & Attachments
Key data trapped in documents no one has time to read at intake
Manual Entry
Repeated re-keying introduces delays and errors on every claim
No Priority Signal
Every claim enters the queue the same way — urgency only visible after manual review
After
Structured FNOL Intelligence
Structured Intake
Loss type, severity, coverage flags — extracted and validated automatically. No missing fields.
Document Processing
Policies, photos, and reports processed at intake — key data surfaced before the adjuster opens the file.
Decision-Ready Signals
Routing recommendation and severity score ready on arrival. Adjuster calls once — with everything.
Priority Queue
Complex claims flagged immediately. Simple claims fast-tracked. No manual triage needed.
Intake that used to take 15–25 minutes of manual effort — structured and decision-ready in under 2 minutes.
Deploy Anywhere
Run Bitligence's FNOL AI on your infrastructure of choice—whether cloud or on-premises.
Amazon Web Services
Microsoft Azure
Google Cloud Platform
On-Premises
Cloud-agnostic architecture designed for security, compliance, and control. Deploy FNOL AI where your data lives—whether that's AWS, Azure, GCP, or your own data center.
How a Pilot Actually Works
No long kick-off. No IT project. No commitment until you've seen it work.
1 session
Map the Intake Gap
We review your current FNOL flow, channel mix, and where adjusters lose time to identify the single workflow where structured AI intake will have the fastest impact.
One working session. No data required yet.
2 weeks
Run It on Real Claims
We process a sample of your actual FNOL input — voice transcripts, web forms, or whatever comes in first — through the intake agent in your environment.
Your data stays in your perimeter. Your IT team stays out of it for now.
2 weeks
Compare Against Your Baseline
We compare what adjusters received before versus after and measure what actually matters: touchpoints, time to route, and data completeness at first notice.
You define what better looks like. We prove it against that.
Your decision
Expand or Exit — Your Call
If the numbers move, we build from there. If they do not, you leave with a clear diagnosis of where intake is leaking and no contract to unwind.
Most pilots reach Step 4 in 6 weeks.
Built for claims operations that need results, not roadmaps.
Not sure if AI is worth it?
Let's share real insights.
We don't sell dreams — we share data.
STRATEGIC INSIGHTS
Download Research‑Backed Briefs
Concise, carrier‑grade insights you can share internally.
From the Founder
I've spent years working inside claims operations — and I've seen where AI initiatives actually break down. Not in the models, but at the very first step. Messy intake. Unstructured data. Manual validation. That's where delays begin and where downstream inefficiencies compound.
I've built these systems at scale — including a voice platform handling over 20,000 FNOL calls a day at a top-tier national carrier. I know where the data breaks down and what it costs when it does.
Small and mid-size carriers feel this most. They carry the same claims volume and the same adjuster friction — without the large internal AI teams of the nationals.
I started Bitligence to fix that first step. Turning FNOL into structured, decision-ready intake using agentic AI — with responsible AI governance built in from the start. Using your data. Clear outcomes. No large upfront commitment.
We start where claims actually break.
FAQs
The questions carriers ask before starting a pilot — answered directly.
Yes — and that's not an afterthought. It's the architecture. Every routing decision Bitligence makes is logged with a rationale. Every PII field is detected and masked before it touches a downstream system. Every output is auditable — model version, policy version, and the reason for each classification are all on record. If a regulator asks why a claim was prioritized the way it was, you have the answer. Most intake systems can't say that. Bitligence is built specifically for environments where that answer has to exist.
No. Bitligence sits upstream of your claims management system — before data enters Guidewire, Duck Creek, or whatever platform your adjusters work in. It processes the unstructured input at first notice and hands your existing system structured, enriched data. No replacement. No migration. No IT project to start a pilot. The integration question comes later — after you've seen it work.
Six weeks, end to end. Week 1: We map your intake flow and identify the highest-impact workflow to test. Weeks 2–3: We run the intake agent on a sample of your real FNOL input. Weeks 4–5: We measure the output against your current baseline — adjuster touchpoints, routing accuracy, data completeness at first notice. Week 6: Results review. You decide what's next. No long kick-off. No IT involvement required for the pilot phase.
You leave with something more useful than a failed pilot — a clear diagnosis of exactly where your intake is leaking and what it's costing you in LAE and cycle time. No contract to unwind. No 12-month commitment to exit. The pilot is designed to produce a clear answer in either direction — and both answers have value. Most carriers who don't move forward still use the intake gap analysis internally. That's intentional.
Your data stays in your perimeter. Bitligence deploys on Azure within your environment — data doesn't move to an external system during the pilot. Access during the pilot: your team and one Bitligence implementation contact. That's it. PII is detected and masked at ingestion — names, phone numbers, addresses are flagged and handled before anything is logged. The audit trail records decisions, not claimant data.
FNOL intake — specifically the gap between first contact and adjuster assignment. That's where unstructured data causes the most downstream friction, where routing decisions are made without enough signal, and where a 6-week pilot produces the clearest before/after result. It's also where Bitligence requires the least IT involvement to test. You don't need an integration to run a sample through the intake agent and compare the output to what your adjusters are receiving today.
No. It feeds them better data. Bitligence processes the unstructured FNOL input before it reaches your claims management system. What enters Guidewire or Duck Creek is already structured, severity-scored, routed, and enriched — instead of a free-text note and a blank priority field. It's not a replacement. It's the layer that makes what you already have work the way it was supposed to.
See how FNOL AI improves claims workflows — with a structured, low-risk approach.



